The liver is a vital organ. Located in the upper right-hand part of the abdomen, it is the largest organ in the body. It’s comprised of two dark reddish-brown lobes.
Think of this organ as a chemical factory. Nutrients absorbed from the digestive tract then metabolize thanks to this football-sized organ. Later, they release into the general circulation. The liver also metabolizes toxins, either ingested or produced by the body. Finally, it manufactures many essential molecules that release into the blood, like clotting factors.
What Causes a Toxic Liver?
Most people never think about their liver. It just quietly goes about its business, never hurting or drawing any attention to itself. The liver has impressive regenerative capacities. In fact, it can re-grow an entirely new organ from just a small fragment of itself.
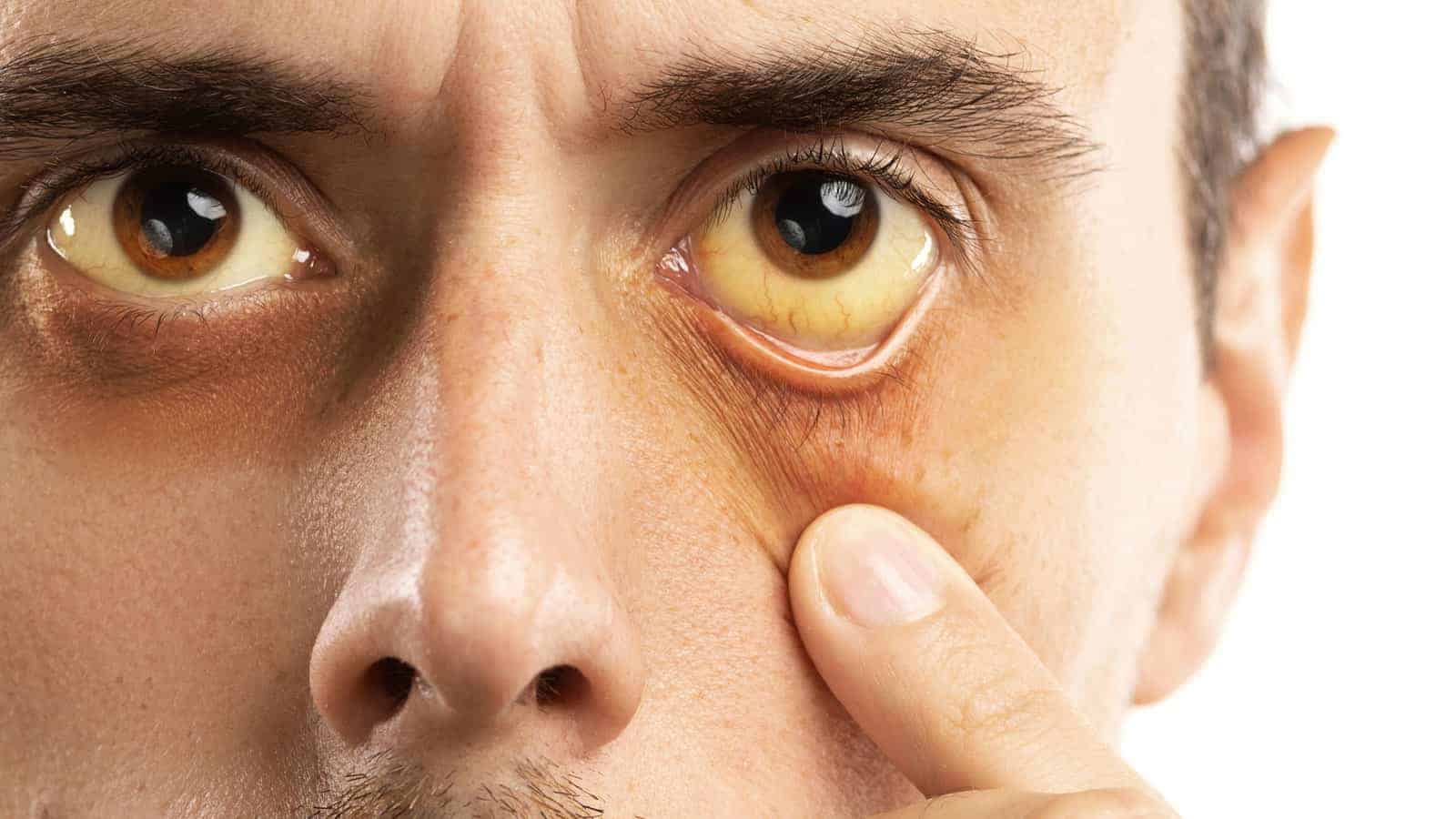
However, some chronic conditions can, over time, damage the organ to the point it begins to fail. Although the classic symptom of a toxic liver is jaundice (turning yellow), this hepatic dysfunction only happens when the condition is relatively advanced.
Common causes of hepatic damage
- Hepatitis or other infection
- Autoimmune conditions
- Iron buildup from hemochromatosis
- Cancers
- Chronic heavy drinking
- Chronic exposure to toxins such as those found in some dietary supplements
- Nonalcoholic fatty liver disease (NAFLD)
Most people have heard of all of these conditions except the last one, NAFLD. However, NAFLD is becoming increasingly common in western societies and is currently the number one cause of chronic hepatic dysfunction in the US. It is characterized by a buildup of fat in the hepatocytes. Its roots are not entirely clear, but it links to obesity, high blood sugar, and high levels of triglycerides in the blood.
NAFLD can progress to nonalcoholic steatohepatitis (NASH), which in turn can progress to cirrhosis and complete organ failure. Advanced symptoms of NASH include abdominal swelling, enlarged, visible blood vessels, jaundice, and red palms.
Another often overlooked cause of hepatic dysfunction is dietary supplements. Many people make the huge mistake of thinking “natural=safe,” which is very untrue. For example, the death cap mushroom is as natural as you can get, but if you consume it, it will irreversibly destroy your organs. Some popular dietary supplements known to cause hepatic damage include:
- Kava
- Pennyroyal oil
- Comfrey
- Mistletoe
- Valerian
- Chaparral
- Skullcap
- Ma-huang
Commonly overlooked symptoms of a toxic liver
1. Itchy skin
If your skin is always itchy and you can’t figure out why, then consider the possibility of a toxic liver. One of the functions of the liver is to get rid of bile salts via the gall bladder. However, if this is not proceeding smoothly, bile salts can accumulate in the skin and make it feel itchy. Of course, many other health conditions can cause itchy skin. Therefore, your doctor needs to investigate the cause thoroughly.
2. Bad breath
Most cases of bad breath arise from problems in the mouth, sinuses, or ears. Sometimes you suffer from this embarrassing condition due to your diet (aka, onion or garlic breath). “Normal” bad breath is referred to as halitosis. Fetor hepaticus is the technical term for a particularly nasty, putrid smell to the breath that originates in your lungs.
Due to the hepatic dysfunction, toxins can build up in your body and expel through your lungs through every exhalation. Many sufferers describe the odor as a combination of rotten eggs and garlic or as a sweetish putrid smell, similar to rotting grass. If you have chronically bad breath, unrelated to your diet, and resistant to oral hygiene efforts, you should schedule an exam right away.
3. Worsening of dark under-eye circles
When most people think of dark under-eye circles, they think of a lack of sleep as the cause. Fatigue can indeed worsen under-eye circles, but they can also be a result of hepatic dysfunction. The dark color under the eye is usually caused by blood vessels under the thin skin in that area becoming dilated and, therefore, more visible. This is why applying a cold spoon to the dark circles after a late night is a time-honored way to remedy the problem quickly; the cold causes the blood vessels to contract.
Problems with toxic liver lead to fluid retention in the body as well as a build-up of toxins and deficiencies of essential molecules and proteins. All of these processes together can lead to dilation of the blood vessels under the eye, making dark under-eye circles much more apparent. These same processes can also make spider veins much more visible on the legs, and advanced disease leads to swelling of the ankles.
4. Excessive sweating
There are many causes of excessive sweating. Surprisingly, a toxic liver is one of them. Most people attribute their increased sweating to hot flashes, wearing too many sweaters, or just environmental conditions and completely overlook this common clue that something is awry internally. These sweaty episodes often mimic menopausal hot flashes in every way, coming on suddenly and causing the sufferer to feel extremely hot, flushed, and well, sweaty. The cause is not entirely clear, but it may be an effort by the body to flush toxins out through the sweat.
5. Fatigue
Fatigue is the most common first symptom of hepatic dysfunction. Still, fatigue is caused by so many other conditions that it is rarely identified as a symptom of a hepatic problem until other symptoms arise. The many functions of the hepatic system cause the entire body to stop working correctly when it starts to malfunction, so it is not surprising that sufferers experience fatigue.
6. Easy bruising
One of the many vital functions of the liver is to produce clotting factors. When hepatic dysfunction occurs, these clotting factors tend not to be delivered in sufficient quantities, which leads to delayed clotting of the blood. Even a minor bump can lead to the formation of a visible bruise. Many people with hepatic dysfunction find they frequently have visible bruises and no recollection of any injury that could have caused the bruising. Some also suffer from spontaneous nose bleeds that take a long time to get under control, again due to the reduced level of clotting factors in the blood.
7. Dark urine
The most common cause of dark urine is dehydration, and the proper response to observing your urine is dark is to reach for some water. However, if your urine remains dark even when you are sure you are properly hydrated, this may be due to a waste product called bilirubin building up in your body and ending up in your urine.
Normally, this product is taken care of by the hepatic system and moves through the digestive tract after passing through the gall bladder. This is the same chemical that turns your skin and eyes yellow or orange when it builds to extremely high levels in the body during advanced hepatic failure.
8. Constipation
Constipation is a common problem in people who consume a typical low-fiber western diet or follow a sedentary lifestyle. You can often relieve this state by simply increasing your intake of fruits and vegetables and getting regular exercise. However, constipation unresponsive to lifestyle changes could indicate a serious health problem, such as a toxic liver or colon cancer.
So, it’s embarrassing to discuss your stools. But rest assured, you should consult a doctor if you develop persistent constipation that doesn’t respond to simple lifestyle changes.
Diagnosis
A standard workup for a possible hepatic issue generally includes a basic physical examination and blood work. The blood levels of two enzymes, in particular, aspartate aminotransferase (AST) and alanine aminotransferase (ALT), are excellent markers of hepatic damage. Elevated AST indicates damage to several different organs, including the heart, but elevated ALT is specific to hepatic injury. These blood tests cannot determine the extent of hepatic dysfunction or determine its cause.
Thus, if doctors find elevated AST and ALT, they usually investigate the issue further. For example, imaging tests of the abdomen with ultrasound, CT, or MRI may be conducted. A final diagnosis of the cause of hepatic dysfunction may require a biopsy, where a long needle is inserted into the organ to collect a sample of tissue.
 Final Thoughts: Treatment for a Toxic Liver
Final Thoughts: Treatment for a Toxic Liver
Treatment depends entirely on the cause of the condition and its severity. For example, doctors will usually treat cases of hepatitis caused by viral infections with antiviral agents. But they’ll treat other conditions, such as NAFLD, by lifestyle changes, such as losing weight, controlling blood sugar, and making dietary changes. Unfortunately, the only treatment for advanced cirrhosis is a transplant. And that is why you should visit your physician to detect a toxic liver as early as possible. Then, you can receive treatment for the problem before it progresses to cirrhosis.













 Community
Community

