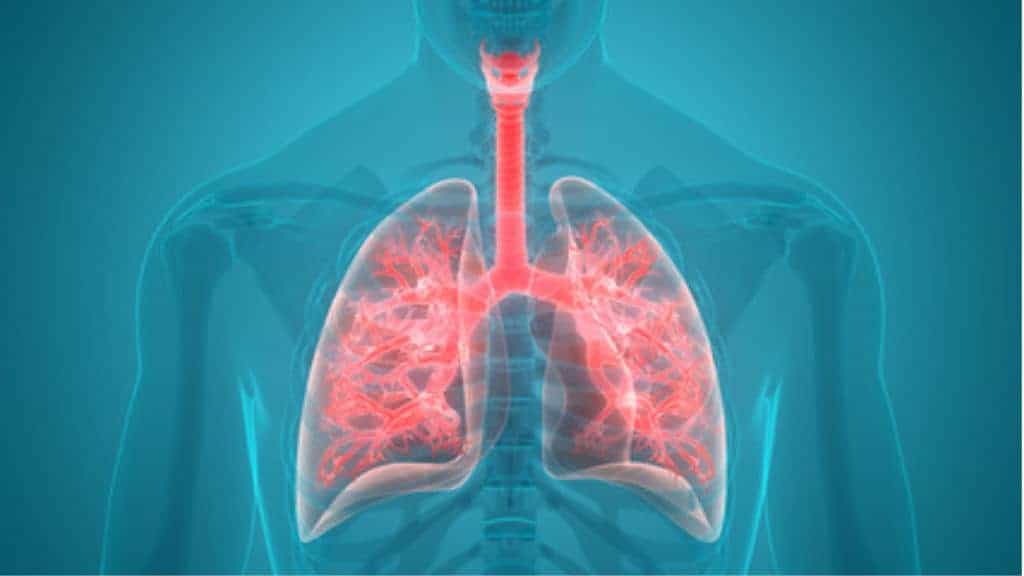
Pneumonia is a common infection that causes inflammation in the air sacs of one or both lungs. The inflammation causes mucus and other fluids to accumulate in the air sacs.
Pneumonia can be relatively mild, but it can also be deadly. The infection is particularly dangerous to people who are under two years old or over 65 years old. It is too dangerous for people with weakened immune systems or other health problems.
Where Do People Pick Up This Illness?
The infection is often categorized by where or how the patient contracted it. In 2019, the National Center for Biotechnology Information (NCBI) published an overview describing the different categories. Most cases are described as “community-acquired,” which means the patient wasn’t in a hospital or other health care facility when they got sick. Community-acquired infections are the eighth most common cause of death in the United States.
A person can also contract the disease in a hospital or similar facility. This infection happens because the patient is already ill. To make matters worse, the bacteria involved are often resistant to antibiotics. The patient is said to have contracted the disease in the hospital if they fall ill at least 48 hours after admission.
People with cancer have an exceptionally high risk of contracting infections in general. Not only are they already ill, but chemotherapy kills healthy cells along with cancer cells. It thus damages the immune system, and it will take the patient time to recover from the treatments.
Ventilator-associated pneumonia (VAP) describes any infection that develops at least 48 hours after a patient has undergone endotracheal intubation.
A patient may also get ill through aspiration, in which they swallow something, and it goes down the wrong pipe and into their lungs. The substance then causes inflammation in the bronchial tubes and the lungs. Large amounts of gastric juices can cause the patient to suffer acute distress in under an hour.
Causes of Pneumonia
1. Bacteria
In 2019, the National Center for Biotechnology Information published an overview describing bacterial infections, as they cause the most severe symptoms and most fatalities. They are also frequent; there are over five million cases of community-acquired lung infections alone in the US every year. Eighty percent of these receive outpatient treatment for the illness.
Streptococcus pneumoniae is the most common cause of bacterial infections in the United States, and it is particularly common in the community-acquired type. It can develop on its own or after the patient has had an upper respiratory infection like a cold. The bacteria may cause a condition called lobar pneumonia, which is confined to one lobe or part of a lung. Other bacteria that can attack the lungs include Klebsiella pneumoniae, Staphylococcus aureus, Pseudomonas aeruginosa, Legionella pneumophila, and Hemophilus influenza. Patients in hospitals may also contract Gram-negative bacteria like Enterobacter or Escherichia coli.
Risk factors for bacterial infection include a weak immune system, old age, illness, and poor nutrition. Patients who have recently had surgery, smoke, or drink too much also have an increased risk of contracting a bacterial infection.
2. Bacteria-like Organisms
Mycoplasma is a genus of bacteria-like organisms that don’t have cell walls and are often resistant to antibiotics. M. pneumoniae often causes “walking pneumonia,” which is usually mild enough that the patient doesn’t need bed rest.
The Journal of Clinical Medicine, however, described a 2018 study in which researchers found that M. pneumoniae can kill particularly vulnerable patients. The scientists studied 203 patients who had been admitted to the hospital. Sixteen of them died. The researchers found that the deceased patients were typically over 65 years old and often had obstructive airway disease (OAD) or weakened immune systems.
3. Fungi
Fungal infections most commonly occur in people with compromised immune systems or chronic health problems. They can also occur in people who have inhaled large amounts of spores. The type of fungus varies depending on the location, and the spores are often found in bird droppings or soil. Pneumocystis carinii is one fungal species that can infect the lungs, but it is never found in healthy people. In North America, the most common genera of fungi are Blastomyces, Coccidioides, and Histoplasma.
4. Viruses
The same viruses that cause flu and colds can sometimes cause pneumonia. Viral infections cause about 50 percent of cases, but they are most common in children younger than five years old. Fortunately, they are usually relatively mild. Unfortunately, a viral infection can sometimes lead to a more serious bacterial infection. Typical viruses include adenoviruses, parainfluenza virus, and respiratory syncytial virus.
First Signs of Pneumonia
1. Chest Pain
A sharp and stabbing chest pain is one of the first symptoms. Pneumonia has four stages: consolidation or congestion, red hepatization, grey hepatization, and resolution. Consolidation takes place during the first day of illness. During this stage, white blood cells attack infectious agents and cause inflammation. Fluid fills the alveoli (air sacs) in the lungs, and the infection soon spreads to other parts of the lung. The patient develops chest pain that is exacerbated by breathing.
2. Cold-like Symptoms
Many early symptoms resemble those of the common cold. The patient will have a scratchy or sore throat and may also feel unusually tired. Later on, they will develop a congested nose, a cough, and a headache. One difference between a cold and pneumonia is duration; the latter lasts longer. If cold-like symptoms show no signs of getting better after three to five days, it’s time to call the doctor.
3. Cough That Can Produce Phlegm
Coughing is another symptom that appears during the consolidation stage. A patient with viral infection may not cough up any phlegm, while a patient with a bacterial infection will often cough up colored phlegm. In fact, a cough that produces mucus is the most common symptom. A patient with a bacterial infection should call their doctor, as an untreated bacterial infection can cause lung damage.
4. Shortness of Breath
Difficulty breathing is another early symptom. It often accompanies rapid breathing. In some cases, the fluid will accumulate between the chest wall and the lungs, which makes breathing even more difficult. The infection can also cause inflammation of the pulmonary pleura, which is the lining on the exterior of the lungs.
A doctor will generally start with a physical exam during which they will listen to your lungs with their stethoscope. They will order an X-ray to determine the location and extent of the infection. They may also request an ultrasound to look for abnormalities on the exterior of the lungs. Lab tests, like those of blood or phlegm, will help the doctor identify the type of microorganism made you ill so that they can prescribe the appropriate medications and treatments. Antibiotics won’t help you if you have a viral infection, for example, but they could be precisely what you need if you have a bacterial infection.
5. Fever, Sweating, and Chills
A temperature indicates that your body is trying to fight off an infection caused by hostile microorganisms. A fever is particularly dangerous if it reaches above 103 degrees Fahrenheit. Such a high temperature can be life-threatening if it is not swiftly treated.
Fevers don’t always cause people to sweat; different people respond differently to abnormally high temperatures. Some people experience intense chills that make them shiver.
In most cases, patients suddenly develop a high fever that is often accompanied by chills. It may take them only a few hours to start feeling very sick. Some patients, however, may develop symptoms gradually, especially if they are older.
If untreated, the fever can last for a week. As the body’s temperature returns to normal, the patient will often sweat profusely. The blood vessels in the skin dilate to help the body get rid of excess heat. Unfortunately, that can strain the circulatory system and heart, especially if the patient has a chronic condition. Consequently, the patient may develop complications after their fever starts declining.
6. GI Tract Symptoms
These can include abdominal pain, diarrhea, nausea, and vomiting. These symptoms can develop quite early in children – to the point that their parents will take them to a doctor to be treated for a stomach problem. In 2011, the European Respiratory Journal described a study in which scientists worked with 258 children between 3 and 14 years old. Many of the children had acute pain in the abdominal area – and it was the first symptom in 22 of them. The scientists found that some of the children had symptoms that mimicked those of appendicitis. Treating the children’s pneumonia caused their stomach pain to clear up.
Final Thoughts on Identifying the Signs of Pneumonia Early
Since pneumonia can be fatal, you should contact your doctor if you suspect that you or someone in your family has it. While the fungal types are not contagious, the bacteria and viral forms are. When somebody with a bacterial or viral infection sneezes or coughs, they send tiny droplets containing the contagion into the air – and anybody nearby could inhale those droplets and thus contract the infection.
If you have a bacterial infection, you will remain infectious until around the second day after your course of antibiotics. If you contracted a viral infection, you would remain infectious until you have been fever-free for several days.
It can take weeks to recover fully, so you should get plenty of rest and follow your doctor’s instructions.