Do you suspect you are suffering from an allergic condition called hay fever?
According to the American College of Allergy, Asthma, and Immunology, more than 50 million people in America are struggling with allergies of some kind. And hay fever is one of them. For those who are not familiar with this type of allergy, hay fever stems from inflammation in the nose that occurs when the immune system encounters and overreacts to allergens in the air. Estimates indicate that 18 million Americans struggle with hay fever, which is often either seasonal or perennial. Those who develop this type of allergy often find themselves confronted with symptoms that can make healthy day-to-day living difficult.
13 EARLY SIGNS OF HAY FEVER
In many cases, those who struggle with hay fever often don’t realize that their symptoms are related to an allergic reaction. For the most part, hay fever symptoms are not too dissimilar from that of the common cold. To help put this into perspective, let’s take a look at 13 early signs of this specific type of allergy. Whether an individual develops seasonal or perennial allergic rhinitis, also known as hay fever, they will typically experience the following:
- Nasal congestion
- Sneezing
- Runny nose
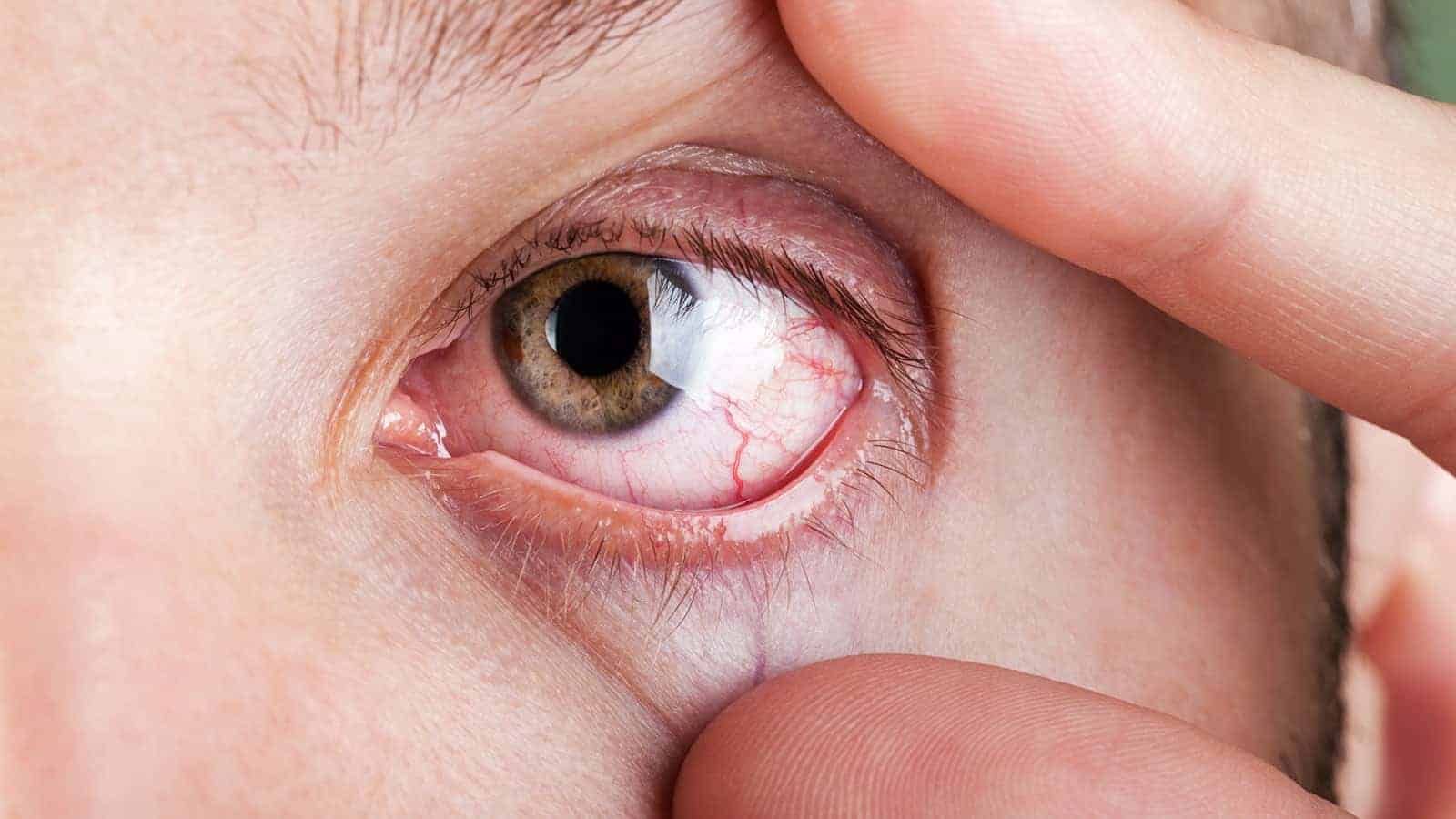
- Watery, red, and itchy eyes
- Postnasal drip
- A chronic cough
- Sinus pressure
- Sinus pain
- An itchy throat
Along with these symptoms, individuals with severe allergic rhinitis may also experience the following:
- Profuse sweating
- Headaches or migraines
- A loss of taste and smell
- Facial pain
It is also not uncommon for those struggling with hay fever to find themselves having to contend with bouts of fatigue, insomnia, and irritability, all of which makes matters even worse. Also, those who have respiratory problems, such as asthma, the condition may trigger wheezing and may even leave them feeling breathless.
WHAT ALLERGENS TRIGGER ALLERGIC RHINITIS?
Now that we are more familiar with allergic rhinitis and some of the symptoms associated with the condition. Let’s take a look at some of the allergens in the air that may contribute to it. Of course, it is worth noting that not everyone will experience an allergic reaction to the same allergens. That said, some of the most common allergens that trigger allergic rhinitis symptoms include
- Fungi and mold spores
- Pet dander
- Pet hair
- Perfumes and colognes
- Dust mites
- Pollen
It is worth noting that exposure to these allergens can trigger an allergic response whether an individual is indoors or outdoors. In either case, once the exposure happens, the immune system will identify these substances as a threat to one’s bodily health. From there, it will produce antibodies that signal blood vessels in the body to expand to facilitate the flow of histamine, the inflammatory chemical responsible for many of the allergy symptoms detailed in this article.
WHO IS MOST LIKELY TO STRUGGLE WITH ALLERGIC RHINITIS?
Exposure to fungi, mold, pet dander, and pollen, for example, will trigger a mild allergic response in most people. However, some people are genetically predisposed to develop acute allergic rhinitis when they encounter them. In short, if an individual’s parents or siblings are struggling with allergic rhinitis, their chances of struggling with it themselves will be quite high. And this claim is substantiated by a study published by the National Institutes of Health, which examined both the environmental and genetic causes of allergic rhinitis.
ENVIRONMENTAL FACTORS THAT CAN MAKE ALLERGIC RHINITIS WORSE
Although symptoms associated with allergic rhinitis are unpleasant, they can be made worse by several environmental factors, some of which include
- Air pollution
- Aerosol sprays
- Humidity
- Tobacco smoke
- Wind
- Changes in temperature
All in all, poor weather conditions and environmental irritants can further inflame the delicate lining of tissue in the nose, which makes allergic rhinitis-related symptoms even worse. That said, if you have allergic rhinitis, it would be best to limit your exposure to poor weather and environmental irritants as much as possible. In doing so, you will prevent your symptoms from spiraling out of control.
HOW IS ALLERGIC RHINITIS DIAGNOSED?
If you’re experiencing any of the symptoms mentioned in this article after being exposed to indoor or outdoor allergens, there is a strong possibility that you have allergic rhinitis. However, to confirm that is, in fact, the case, you will want to schedule an appointment with an allergist. During your exam, your physician will inquire about the specific symptoms you’re experiencing. He or she may ask about your family and personal medical history as it pertains to allergies. To confirm your symptoms allergic rhinitis-related, your physician will likely start by ordering a blood test.
WHAT WILL A BLOOD TEST REVEAL?
While the prick-like sensation caused by the needle used to draw your blood might only last for a few seconds, the blood test itself can take 15 to 20 minutes. The blood sample is then sent to a laboratory to be examined. And from there, laboratory technicians will measure the level of IgE antibodies. If the level of IgE antibodies measures six or higher, it generally indicates that the blood contains allergens. In most cases, a blood test will also reveal the specific allergen that is triggering a patient’s symptoms; however, sometimes, a skin-prick test might be needed as well. The test involves the physician injecting known allergens into a patient’s skin and then waiting about 20 minutes to see whether or not they develop an allergic reaction.
WHAT TREATMENTS ARE AVAILABLE TO THOSE STRUGGLING WITH ALLERGIC RHINITIS?
If you’re struggling with allergic rhinitis, know that you can find many over-the-counter and prescription-based treatments to relieve your symptoms. Some of these medical treatments include the following:
OVER-THE-COUNTER TREATMENTS FOR HAY FEVER
Antihistamines
Over-the-counter antihistamine sprays and tablets are highly effective when it comes to relieving most allergic rhinitis-related symptoms, such as a runny nose, itching, and sneezing. Some of the go-to medications for many people include Allegra, Benadryl, Claritin, and Flonase Nasal Spray.
Eye drops
Because watery, red, itchy eyes are often par for the course when it comes to allergic rhinitis, many allergists will advise their patients to take over-the-counter eye drops that contain sodium cromoglycate. This active ingredient is available in several over-the-counter eye drops, including Opticrom, and works by inhibiting the release of histamine that can irritate the eyes.
PRESCRIPTION-BASED TREATMENTS
Those with severe allergic rhinitis-related symptoms should seek care from a licensed physician. Some of the most common prescription-based treatments include
Immunotherapy
This physician-prescribed treatment is ideal for most people as it offers long-term symptom relief. Immunotherapy, also known as allergy shots, works by helping the immune system become desensitized to allergens over time. For most allergies, including allergic rhinitis, allergen immunotherapy is successful in nearly 80 percent of cases, according to a study published by the National Institutes of Health. In short, allergen immunotherapy entails receiving injections that contain a small amount of a known allergen over a long period, which gradually tamps down the allergic response of the immune system. The allergens can also be administered via sublingual drops as well.
Oral corticosteroids
This physician-prescribed treatment, similar to immunotherapy, also provides long-term relief from allergic rhinitis-related symptoms. One of the most commonly prescribed oral corticosteroids is Prednisone. Studies show that this medication helps relieve swelling in nasal passages, which, in turn, restores normal breathing. Prednisone also provides relief from a stuffy, runny, or itchy nose. Lastly, it is highly effective when it comes to assisting sneezing.
Leukotriene receptor antagonists
This physician-prescribed treatment entails taking leukotriene receptor antagonists-based drugs, such as Singulair. This medication, along with other leukotriene receptor antagonists-based pills, works by blocking histamine and other chemicals produced by the immune system that trigger allergy symptoms. It is also considered a go-to pharmacotherapy in the treatment of asthma symptoms that are made worse by allergic rhinitis-related symptoms.
THE NATURAL TREATMENT: PREVENTION IS THE BEST MEASURE FOR HAY FEVER
If you don’t want to take medicines or suffer through a bout of allergic rhinitis, prevent your symptoms! Learn what triggers your flare-ups and avoid them altogether. For some, this means staying indoors with the windows closed on high-pollen count days. And for others, this might mean hiring help dusting and housecleaning.
This prevention, as the adage says, is worth its weight in gold versus the prescription drug so-called “cure.”
FINAL THOUGHTS ON COPING WITH HAY FEVER
In summary, allergic rhinitis can stem from several known allergens. Further, the symptoms associated with this specific type of allergy can range from mild to possibly life-threatening. Once you have identified the allergens that are contributing to your condition, avoid them. Most importantly, if you don’t know what is causing your allergic rhinitis-related symptoms, schedule an appointment and testing with an allergist as soon as possible.
















 Community
Community

