A new study from Imperial College London and the University of South Carolina links high histamine to depression. The findings confirm prior studies that inflammation, which triggers histamine release, affects the hormone serotonin. Low levels of this crucial molecule in the brain seem to link to depression, according to this science.
If scientists can reproduce the study in humans, these findings could lead to new treatments for depression. Depression affects nearly 300 million people worldwide, according to the WHO, although it is likely a conservative estimate. Depression remains the leading cause of disability globally and dramatically contributes to the global burden of disease. It’s believed that this complex mental disorder stems from a combination of social, biological, and psychological factors.
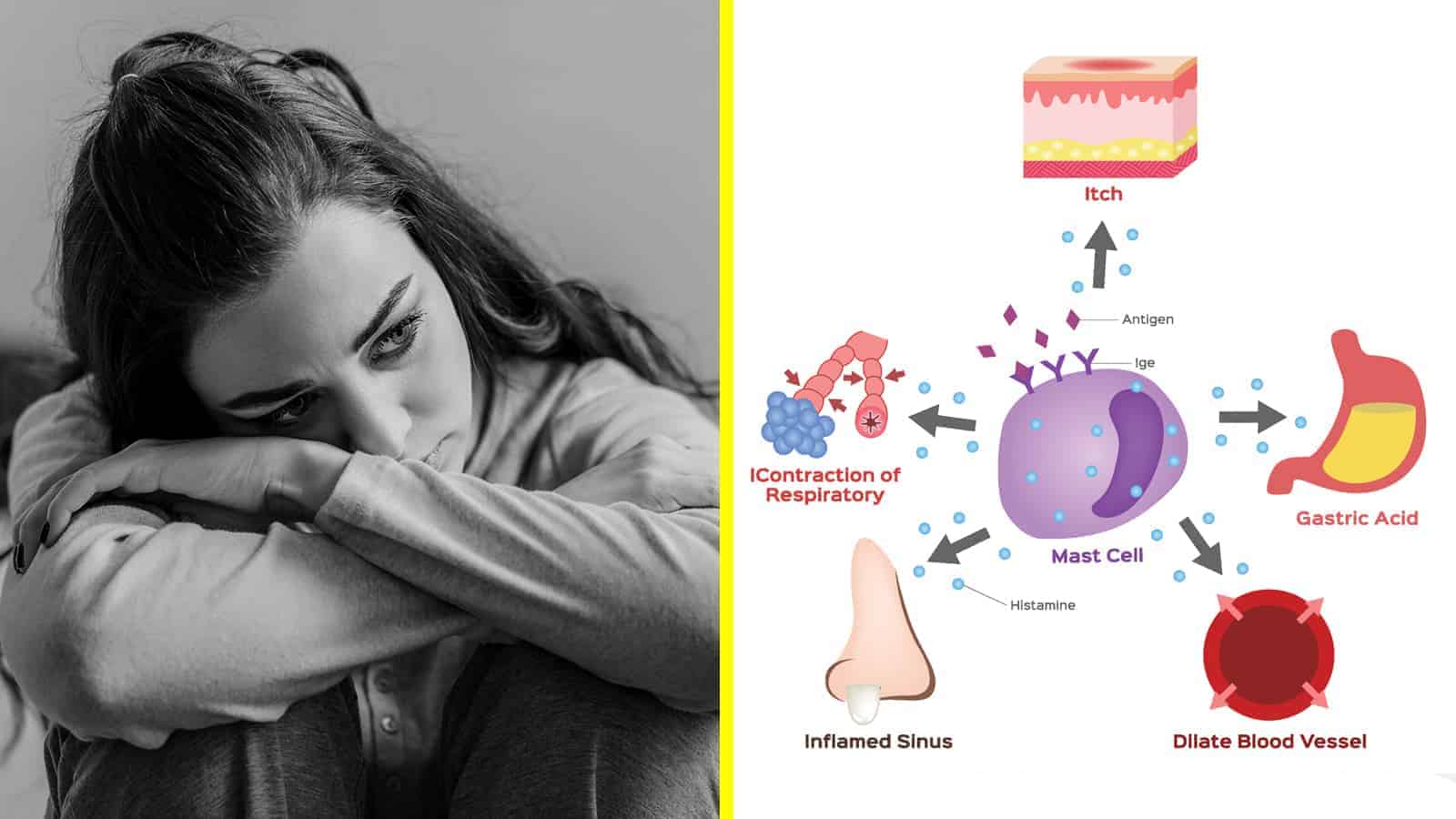
Scientists have attempted to understand the root cause of depression for decades. Now, they reveal how histamine contributes to this devastating mental disorder. The body releases histamine as an immune response to a normally harmless foreign substance, such as pollen. When this happens, immune cells attack the perceived threat, and blood flow increases in affected areas.
How histamine impacts depression
This immune response allows the body to fight infections, but it can become compromised if histamine remains elevated. Chronic inflammation keeps histamine levels high, which weakens the immune system. Many health conditions cause inflammation, including cancer, diabetes, obesity, allergies, and even stress. The study, which appeared in The Journal of Neuroscience, reveals that inflammation-induced histamine might also contribute to depression.
Lead author Dr. Parastoo Hashemi, from Imperial’s Department of Bioengineering, said: “Inflammation could play a huge role in depression, and there is already strong evidence that patients with both depression and severe inflammation are the ones most likely not to respond to antidepressants.
“Our work shines a spotlight on histamine as a potential key player in depression. This, and its interactions with the ‘feel-good molecule’ serotonin, may thus be a crucial new avenue in improving serotonin-based treatments for depression.”
How serotonin impacts histamine in the body
Many antidepressants target serotonin, commonly called the “feel-good hormone.” Most selective serotonin reuptake inhibitors (SSRIs) impede the re-absorption of serotonin in the brain. This allows the serotonin to circulate for a more extended period, enhancing mood and warding off depression.
SSRIs undoubtedly improve many lives, but an increasing number of people have become resistant to their effects. Experts believe that specific interactions between neurotransmitters, including serotonin and histamine, play a considerable role in treatment-resistant depression.
So, researchers focused their investigation on the complex relationship between histamine, serotonin, and SSRIs. For the study, they placed microelectrodes in the hippocampus of the brains of live mice to measure serotonin levels. The hippocampus helps regulate mood and plays a vital role in storing and recalling memories.
This method, also called fast-scan cyclic voltammetry (FSCV), allowed them to measure serotonin levels without harming the brain. The microelectrodes measure only five micrometers wide and do not endanger living tissue. After placing the microelectrodes, they gave half the mice lipopolysaccharide (LPS) injections, a toxin found in some bacteria that triggers inflammation. Scientists gave the other half, the control group, a saline solution.
The observations
The researchers observed that brain serotonin levels decreased after a few minutes of the LPS injection. In the control mice, serotonin levels did not change. This shows how quickly the brain responds to inflammation, which affects serotonin levels. Since LPS cannot cross the blood-brain barrier, it couldn’t have been responsible for causing the decrease in serotonin.
Upon investigating further, the researchers found that the inflammation triggered the release of histamine, which directly inhibited serotonin. This occurred when the histamine attached to inhibitory receptors on the serotonin neurons. Scientists believe a human study would reproduce this effect since humans also have these receptors on their serotonin neurons.
To see how SSRIs would affect histamine and serotonin, researchers administered them to the mice. Surprisingly, the control mice had higher serotonin levels than the other group. Researchers believe this occurred because the SSRIs caused histamine levels to rise, which canceled the serotonin boost.
Next, researchers gave the mice antihistamines to counter histamine’s inhibitory effects. This caused serotonin levels to rise back to normal levels. The findings confirm the scientists’ theory that histamine directly inhibits serotonin in the brain. The histamine-reducing drugs triggered a whole-body drop in histamine, unlike regular antihistamines taken for allergies, which only affect neurons.
Histamine: A new molecule of interest in depression treatment
Researchers say that if they can replicate the study in humans, it could lead to better depression treatments. Doctors could measure chemicals like serotonin and histamine in human brains to more effectively target and detect depression. The study authors added that the findings might result in new opportunities to explore histamine’s role in depression. Perhaps the research would prompt the development of improved medications to reduce histamine in the brain.
Since the study only involved mice, researchers will need to observe the effects in humans moving forward. However, the fact that they can’t use microelectrodes in human brains may act as a roadblock. They’re currently researching other techniques to get a glimpse of the human brain. Scientists believe the gut may help them continue their studies since it also synthesizes serotonin and histamine.
The researchers also said that pain, which accompanies inflammation, can trigger changes in neurotransmitters. However, prior research shows that these changes only last a few minutes. In this study, the decrease in serotonin lasted much longer, proving that pain didn’t cause the serotonin drop.
Dr. Hashemi added: “Inflammation is a whole-body response and is therefore hugely complex. Depression is similarly complex, and the chemicals involved are affected in myriad ways by both genetic and environmental factors. Thus we need to look at more complex models of depression behaviors in both mice and humans to get a fuller picture of both histamine and serotonin’s roles in depression.”
Final thoughts on a study linking histamine to depression
Scientists have been studying the causes of depression for years to help improve treatments. They’ve recently discovered that histamine, a chemical messenger involved in the immune response, plays a crucial role in depression. Chronic inflammation, which elevates histamine, causes serotonin levels to drop. Low levels of this critical hormone have been strongly associated with depression.
The study offers promise for improved depression treatments that target histamine. In combination with SSRIs, this could provide an answer for people with treatment-resistant depression.















 Community
Community

