Colon cancer is a devastating disease.
It is one of the most common types of cancer diagnosed in the US, with around 100,000 new cases diagnosed every year. It is also one of the most common causes of death from cancer in the US. However, due to colonoscopy and improvements in treatment, the incidence and mortality rate of colon cancer has been steadily decreasing over the past few decades. Currently, cases identified in the early stages have a 90% survival rate. Unfortunately, cases identified in the late stages have only a 14% chance of surviving.
Treatment primarily involves surgery to remove the tumor followed by chemotherapy and/or radiation. If the cancer is large, a surgeon might remove a significant portion of the colon or rectum. Therefore, some patients require a permanent colostomy bag after treatment. There are also a number of targeted therapy drugs available that are active against colorectal cancer and may be used to help treat advanced forms of the disease.
This cancer arises from the epithelial cells that line the interior of the colon or rectum. You’ll also hear the condition called colorectal cancer. Medically, the term “colon” refers to the large intestine. It connects the small intestine to the rectum, which then empties through the anus. Its primary role is to extract the remaining nutrients and water from the digested food and to form and store stool until it passes.
Additionally, it serves as the primary home of your all-important gut bacteria, which ferment fiber, generate vitamins and other nutrients, and can affect the health of your entire body and even your emotions.
The role of colonoscopy
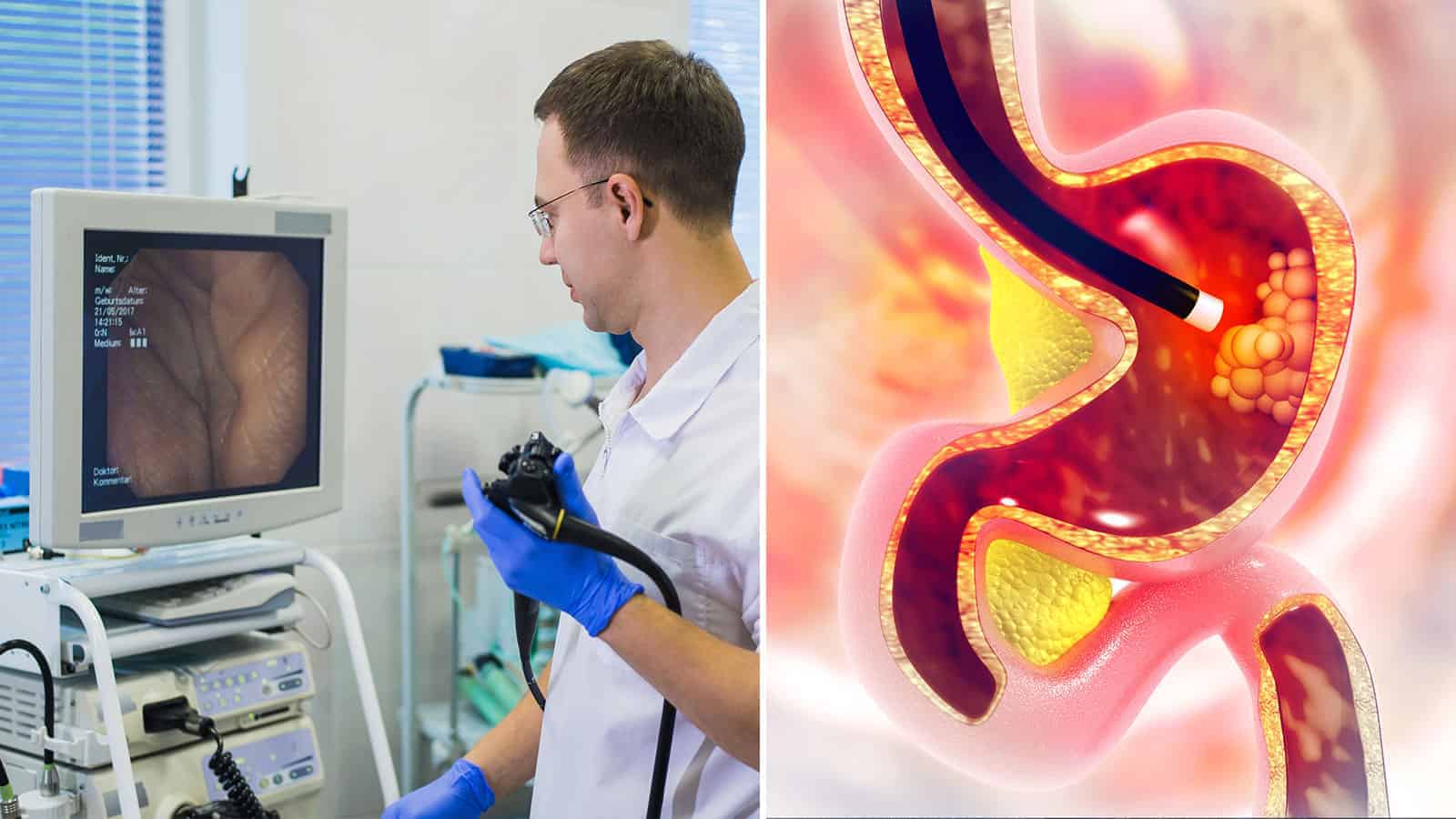
Colonoscopy is a minimally invasive method that allows doctors to actually look at the interior of the rectum and colon. The physician inserts a narrow tube with a camera on the end through the anus and advances it up the colon. Then, he or she views the appearance of the lining of the colon and rectum on a monitor.Since polyps and cancers look different than normal cells, the doctor can identify them. The scope has a channel that allows the introduction and use of tiny surgical instruments. So, if the doctor can see a polyp, they remove it and collect the tissue. Furthermore, if the doctor finds a growth that appears to be overt cancer, they send the specimen off to a pathologist. That’s a specialty doctor who can determine if it is cancer or just a benign growth.
Screening recommendations
The United States Preventive Services Task Force recommends all adults begin a program of screening for colorectal cancer at age 50. The evidence strongly suggests that people who participate in colon cancer screening programs have a lower incidence of colorectal cancer diagnoses and are far more likely to survive if they are diagnosed with colorectal cancer.
The actual recommendation is rather complicated. That is because there are numerous methods of screening for colorectal cancer, such as fecal occult blood screening, barium enemas, and sigmoidoscopy. Unfortunately, the evidence is not clear as to which method, if any, is superior.
However, one of the recommendations is getting a colonoscopy at age 50 and then every ten years thereafter. Or, have one more frequently if they find a polyp or you have risk factors for cancer. An advantage of using colonoscopy as the primary screening method is if you do have cancer, it can be immediately diagnosed during the screening procedure. And an even more important advantage is if you have a polyp, it can be removed during the screening process and thus prevent cancer from developing in the first place.
How can colonoscopy prevent cancer?
Carcinogenic substances found in food expose the cells lining the interior of the color to carcinogenic substances regularly. Therefore, it is relatively common for them to develop mutations in their DNA. And, since these cells are also constantly dividing in order to form new cells to replace the ones regularly shed into the colon, these mutated cells can easily form small clumps of abnormal cells called polyps. Most polyps never progress to overt cancers, but a certain percentage do.
Unlike some cancers, colon cancer develops very slowly through a well-established and well-studied process of gradual accumulation of mutations and increasingly abnormal cell characteristics. Pretty much every single adenocarcinoma (the most common type of cancer arising from the colon and rectum) slowly develops from a polyp. A polyp is not cancerous; it is an abnormal growth of cells. Most are benign and never progress to cancer, but some do. Colonoscopy can detect polyps during their early stages and simply remove them all. Thus no cancer will ever form from those polyps.
Some people have a genetic predisposition to forming. In addition, these people have a higher risk of developing colorectal cancer. The most usual presentation of this situation is developing two or three new polyps every few years from middle-age onwards. An extreme form of this condition is the inherited FAP syndrome where affected individuals begin growing polyps, often hundreds of them, during their teenage years. These people hold an elevated risk of developing colorectal cancer at a fairly young age. And, in many cases, they opt for surgery to remove their colon or enter into very strict and frequent cancer screening programs.
What is a colonoscopy procedure like?
The actual procedure itself is reported to be “trivially easy” and “uneventful” by most patients. Currently, patients are usually sedated with propofol, which causes them to rapidly fall asleep, remain asleep throughout the procedure, and rapidly wake up, with few to no side effects. The entire procedure takes less than an hour. In fact, some patient procedures take less than 30 minutes if the physician finds no polyps or abnormal tissues.
However, prior to undergoing a colonoscopy, the bowel must be prepped. Namely, completely empty. That allows the doctor to insert the scope and view the color walls clearly. Of course, patients dread this part of the procedure.
The patient follows a special “low residue” diet for a few days. Then they must consume a laxative, to induce the emptying of the colon and rectum. Sometimes the use of an enema is also required. The details of the most common bowel prep procedure are:
- Eat a low fiber diet for three or four days before the procedure
- Consume only liquids the day before the procedure
- Consume the laxative the evening before the procedure
- Stay in the bathroom until the bowel movements stop
- Consume only liquids the day of the procedure
Are there any risks or side effects?
This procedure is routine and is considered to be very safe. There is a very low risk of suffering a bowel perforation, which will require surgical repair if it happens. It’s not uncommon to see a little blood in the stool immediately after the procedure, especially if a polyp has been removed.
What about a virtual CT procedure?
So, it is true that doctors may order a CT machine to look for polyps and possible cancers inside the colon and rectum. However, this procedure has disadvantages. Its primary disadvantage is that physicians cannot sample or remove the polyps. In fact, all they can do is to identify them.
In addition, patients still need to undergo the unpleasant “bowel prep” to provide good views of the lining of the colon. If anything is found during a CT screening procedure, the patient will need to undergo a regular colonoscopy anyway. Thus, simply skipping the CT scan makes the most sense, especially since CT scans also expose the patient to x-rays.
Are there other ways to prevent colorectal cancer?
Diet plays a huge role in altering the risk of colorectal cancer, and unlike genetic predispositions, it can easily be changed to reduce the risk of colorectal cancer. Diets rich in green leafy vegetables, dark-colored vegetables, fruits, and fiber, in general, tend to be protective against cancer of the bowels. Regular consumption of charred, smoked, and preserved meats can increase the risk of cancer of the bowels.
Other modifiable factors that increase the risk of colorectal cancer include the following:
- A lack of exercise
- Being overweight
- Drinking alcohol excessively
- Smoking or use of tobacco.
Taking low-dose aspirin regularly can also lower the risk of colorectal cancer, perhaps by reducing inflammation in the tissues.
Women who take hormone replacement therapy after menopause also have a lower risk of colorectal cancer. However, they should discuss the pros and cons of hormone replacement therapy with the doctor before beginning treatment.
Final thoughts on preventing colon cancer
Colon and rectal cancer are very common in the US, and if patients are diagnosed only when these cancers become symptomatic, namely in an advanced, late-stage, they have very low survival rates, only around 14%. However, if physicians detect these cancers at an early stage through screening, the survival rate increases to 90%.
Currently, the doctors recommend all individuals enter a screening program for colorectal cancer beginning at age 50. The options for screening are diverse and complicated. Therefore, the best option for each individual varies to genetic and lifestyle factors as well as patient preference. And so, you should openly discuss this issue with your doctor before embarking on a screening program.
Thus, the bottom line is that a colonoscopy may detect colorectal cancer in its earlier stages. This test allows physicians to detect and remove polyps before they develop into cancer. And that can save lives.















 Community
Community

