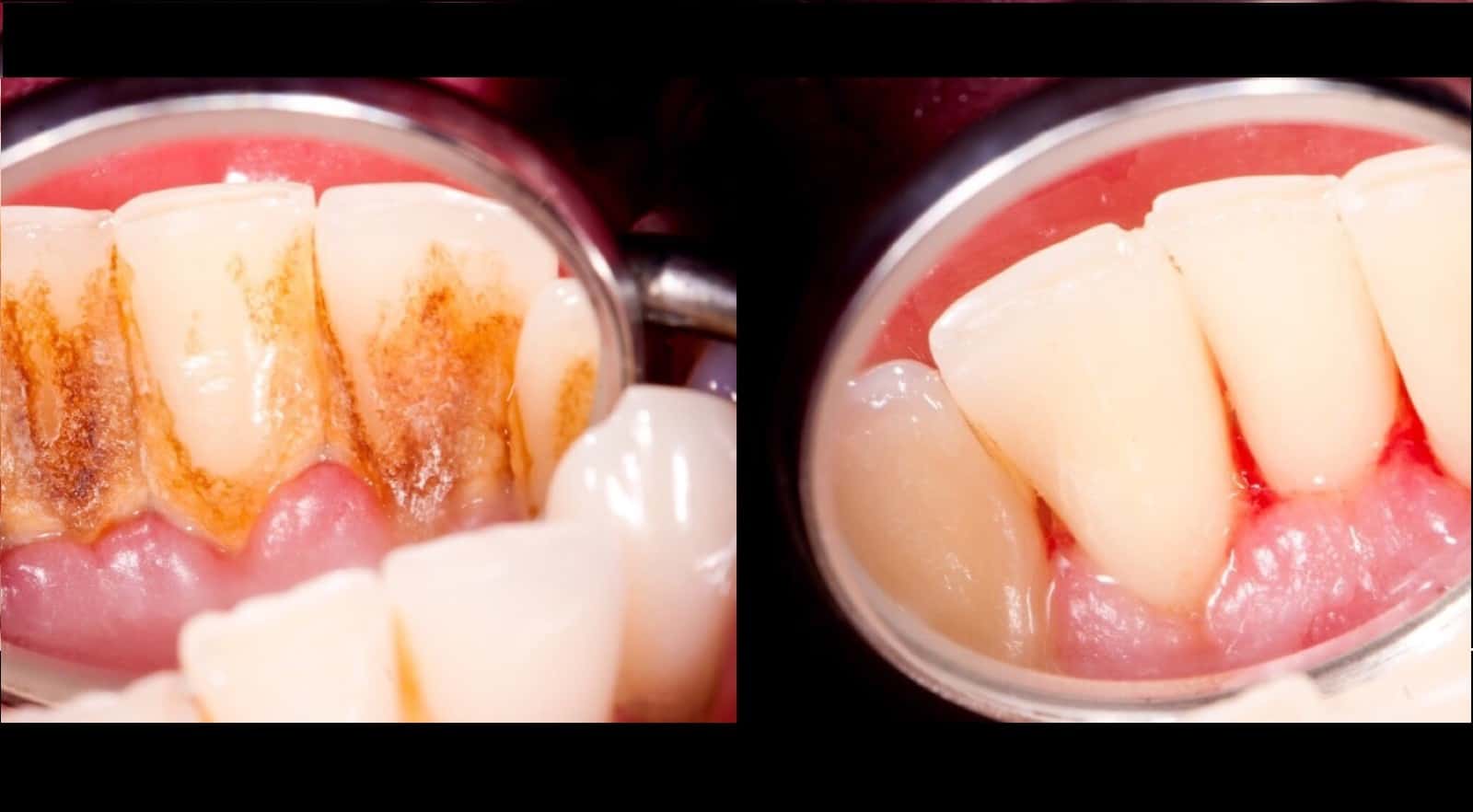
As the name implies, Gum disease is a disease affecting your gums and other surrounding teeth tissues. Also known as periodontal disease, it exists in various types or forms. These diseases usually result from poor oral hygiene. Moreover, understanding the types of periodontal disease can help you prevent it.
In its mildest form, gum disease poses minimal health risks and can be treated quickly and effectively. However, it would help if you did not allow it to progress beyond this early stage. That’s because the condition causes eventual tooth loss and other severe health problems.
Never Ignore These Types of Periodontal Disease
1 – Gingivitis
Gingivitis is the very earliest stage of gum disease. It is pretty mild and easily treated. Any damage to your oral cavity at this stage can be reversed with proper medical care.
What exactly causes gingivitis? Leftover food particles and the bacteria in your mouth form a sticky, soft deposit called plaque on the surface of both your teeth and gums.
The Progression of Gingivitis
If this plaque is not removed by regular brushing and flossing, the bacteria build-up and release harmful toxins. Those irritate and inflame your gums, making them swollen and tender. Aside from gum inflammation, another critical symptom of gingivitis is the tendency for your gums to bleed when flossing or brushing your teeth.
However, it’s crucial to point out that significant damage to your gums or teeth isn’t permanent at this stage. Studies indicate that proper oral hygiene and professional cleaning can reverse your gingivitis and restore your oral health.
2 – Chronic periodontitis
If you don’t detect or treat gingivitis early on, it progresses into a more advanced and dangerous gum disease–periodontitis. If you have periodontitis, spaces or crevices form between your teeth and gums.
These spaces that you develop, called pockets, directly result from your gum and bone pulling away from your teeth. Food particles and other debris enter into these pockets and cause infections. Your body’s immune system immediately seeks to combat these infections and releases enzymes to this effect.
These enzymes eventually do more harm than good as they aggressively produce toxins that help destroy the infected gums and teeth tissues.
The Next Stages of Periodontitis
Your gums begin receding, and your teeth begin appearing longer than usual. Meanwhile, the bacteria in the plaque keep on breeding. Per the Centers for Disease Control and Prevention (CDC), it eventually spreads to areas below your gum line and begins to affect the underlying jawbone.
The pockets formed will eventually become more profound, and the disease worsens quickly. The bacteria also produce their own harmful toxins, which, when coupled with those produced by your body’s immune system, gradually and inevitably destroy your gums, bones, and other teeth, and oral tissue.
Since the disease eventually will kill the tissue anchoring your teeth in place and atrophy your jawbone, your teeth will likely become unstable and need to be extracted.
When gum and bone destruction happens at a slow rate, the gum disease is referred to as chronic periodontitis.
3 – Aggressive periodontitis
Aggressive periodontitis is chronic periodontitis at a much more rapid pace. The transition from gingivitis to periodontitis is relatively fast and aggressive, with gum, bone, and tissue deterioration occurring at a very advanced rate. Ironically, aggressive periodontitis usually affects ordinarily healthy individuals.
Of the two, chronic periodontitis is the most common and occurs most times in individuals above the middle-age bracket. Despite these differences, sufferers of aggressive periodontitis have the same symptoms as those living with chronic periodontitis: receding gums, loose and shifting teeth, and eventual tooth loss.
Most times, the infected pockets between the teeth and gums contain pus. This infection is why most people who suffer from advanced gum disease have chronic bad breath, otherwise known as halitosis, and usually experience a persistent metallic taste in their mouth.
Both forms of periodontitis (chronic and aggressive) involve significant and irreversible tissue damage. However, the progression of these diseases can be halted using specific medical procedures and, if necessary, surgery.
Due to its rapid development, aggressive periodontitis is usually harder to block. A 2014 study shows that treatments consist of antibiotics, surgery, or both.
4 – Periodontitis resulting from systemic diseases
Systemic diseases lower your body’s resistance to infection and make you susceptible to gum diseases. So, if you suffer from systemic diseases such as diabetes mellitus, respiratory diseases, and cardiovascular diseases, your odds of periodontitis increase.
In this case, periodontitis usually results from the underlying systemic disease rather than as a direct consequence of poor oral hygiene. If the systemic disease in question is quite severe, you might face the aggressive form of periodontitis rather than the slower chronic type.
Here, gum disease treatment occurs in two stages. Your dentist must first control the underlying systemic disease. Then, they will implement therapy for periodontitis.
Here’s an essential point to remember. While diabetes, heart, and respiratory diseases are the most common systemic diseases related to gum disease, dozens of other systemic conditions could result in periodontitis. Among those, leukemia and Down syndrome being notable mentions.
Systemic periodontitis is one of those rare gum diseases that can affect young people. It also tends to result in more complicated health problems. It could lead to stroke, and if you’re already suffering from diabetes mellitus or heart disease, your condition worsens.
5 – Necrotizing periodontal disease
People who suffer from HIV, malnutrition, immunosuppression, and chronic stress are more prone to this type of gum disease. Of the five types of periodontal disease mentioned, necrotizing periodontal disease remains the rarest.
If you suffer from this disease, your gums, bones, and other teeth tissues would rapidly die off, leaving noticeable lesions. Unlike other types of this disease, teeth tissues are not destroyed by a bacterial infection. Instead, they are starved of necessary nourishment and die as a result. The term describing the process is necrosis. Unfortunately, it progresses rapidly.
The bottom line on knowing the types of periodontal disease
Although poor oral hygiene remains the most common cause of gum disease, several other factors could lead to this dreaded malady. As earlier established, certain conditions such as diabetes, cardiovascular diseases, and HIV, among others, can increase your chances of contracting gum disease.
Regular consumption of tobacco, vitamin and mineral deficiencies, contraceptive pills, certain medications for blood pressure and seizures, stress, genetic susceptibility, and even hormonal changes such as pregnancy and menopause can also contribute to periodontal disease.
Gum disease treatment is entirely possible with good oral hygiene habits, non-surgical therapy, and more advanced oral surgery cases. To prevent sensitive, bleeding gums, offensive breath, and eventual teeth loss, keep your gums and teeth healthy.
How?
- Brush your teeth at least twice a day.
- Floss at least once daily
- Regularly rinse your mouth with an anti-bacterial mouthwash
- Maintain a well-balanced diet
- Taper down on your smoking habit. Eventually, please quit!
And, most importantly, visit your dentist or dental hygienist for regular check-ups and professional teeth cleanings.