According to Dr. David Majdalani of the Cleveland Health Clinic, there are five symptoms of poor heart health that you should know. So seek immediate medical attention if you experience them.
Five Signs of Poor Heart Health Everyone Should Know
Watch for these red flags and seek advice from your doctor immediately.
1. Abnormal heart beat.
Also known in medical circles as an “arrhythmia”, and it does not necessarily mean your heart is beating too fast or too slow.
This could seem like a skipped beat, an additional beat, some kind of “fluttering”, “tachycardia” – beating too quickly, or “bradycardia” – beating too slowly. Or it may show no symptoms at all, being a “silent” arrhythmia. These could be serious or harmless, so it is best to err on the side of caution and visit your local doctor.
Symptoms of an abnormal heartbeat, according to WebMD:
N.B. There could be no symptoms if it is a “silent” arrhythmia.
– Palpitations – skipping or additional beats, fluttering, or “flip-flops”.
– Pounding in the chest.
– Dizziness.
– Fainting.
– Shortness of breath.
– Chest pain or tightening.
– Feeling very tired – weakness or fatigue.
If you have an abnormal heart beat, stop:
– Doing certain activities that bring on the complaint more often.
– Smoking, if you do.
– Excessive drinking of alcohol. One drink per day for women, two per day for men.
– Excessive intake of caffeine.
– Taking cold and cough medicines containing stimulants. Always seek the advice of your physician to see which medications are optimal for you.
2. Chest pain.
In the words of the NHS in the United Kingdom, “chest pain can be caused by anything from muscle pain to a heart attack and should never be ignored.” However, it might not be the heart that is causing this discomfort. As well as the heart, the pain could be caused by the muscles in the affected area, lungs, gullet, nerves, or ribs, including the sternum. Types of chest pain, as stated on WebMD, include: sharp, dull, burning, aching, stabbing, or a tight crushing sensation.
Symptoms to watch out for in addition to chest pain:
– Dizziness, nausea, fast heart rate or breathing, confusion, grey complexion, or excessive sweating.
– Pain spreading to the jaw, left arm, or back.
– Sudden feeling of pressure or crushing under the breast bone.
– Extremely low blood pressure or heart rate.
– Shortness of breath.
Causes for heart-related chest pain:
– Coronary Artery Disease.
– Angina.
– Heart attack.
– Myocarditis, the same symptoms of a heart attack but without the blockage.
– Pericarditis.
– Hypertrophic cardiomyopathy.
– Mitral Valve Prolapse.
– Coronary Artery Dissection.
3. Deep Vein Thrombosis (DVT).
This is caused by a blood clot in one or more deep veins. This has received media attention over the last decade or two thanks to the deaths of various people from DVT due to inactivity inside aircraft.
It is usually caused when you suffer from “certain medical conditions that affect how your blood clots”, according to Mayo Clinic. It adds that DVT “can also happen if you don’t move for a long time, such as after surgery, following an accident, or when you are confined to a hospital or nursing home bed.” It is known that DVT can also cause a pulmonary embolism, thanks to a free-running blood clot which goes straight to the lungs. A DVT and pulmonary embolism combo is known as venous thromboembolism (VTE).
As noted in the NHS in the UK, symptoms of DVT and pulmonary embolism are:
DVT:
– pain, swelling and tenderness in one of your legs (usually your calf)
– a heavy ache in the affected area
– warm skin in the area of the clot
– red skin, particularly at the back of your leg below the knee.
– DVT usually (although not always) affects one leg. The pain may be worse when you bend your foot upward towards your knee.
Pulmonary embolism:
If left untreated, about one in 10 people with a DVT will develop a pulmonary embolism. A pulmonary embolism is a very serious condition which causes:
– breathlessness, which may come on gradually or suddenly
– chest pain, which may become worse when you breathe in
– sudden collapse
– Both DVT and pulmonary embolism require urgent investigation and treatment.
Risk Factors:
Anyone can develop DVT, but it becomes more common over the age of 40. As well as age, there are also a number of other risk factors, including:
– having a history of DVT or pulmonary embolism
– having a family history of blood clots
– being inactive for long periods – such as after an operation or during a long journey
– blood vessel damage – a damaged blood vessel wall can result in the formation of a blood clot
– having certain conditions or treatments that cause your blood to clot more easily than normal – such as cancer (including chemotherapy and radiotherapy treatment), heart and lung disease, thrombophilia and Hughes syndrome
– being pregnant; your blood also clots more easily during pregnancy
– being overweight or obese
– The combined contraceptive pill and hormone replacement therapy (HRT) both contain the female hormone oestrogen, which causes the blood to clot more easily. If you’re taking either of these, your risk of developing DVT is slightly increased.
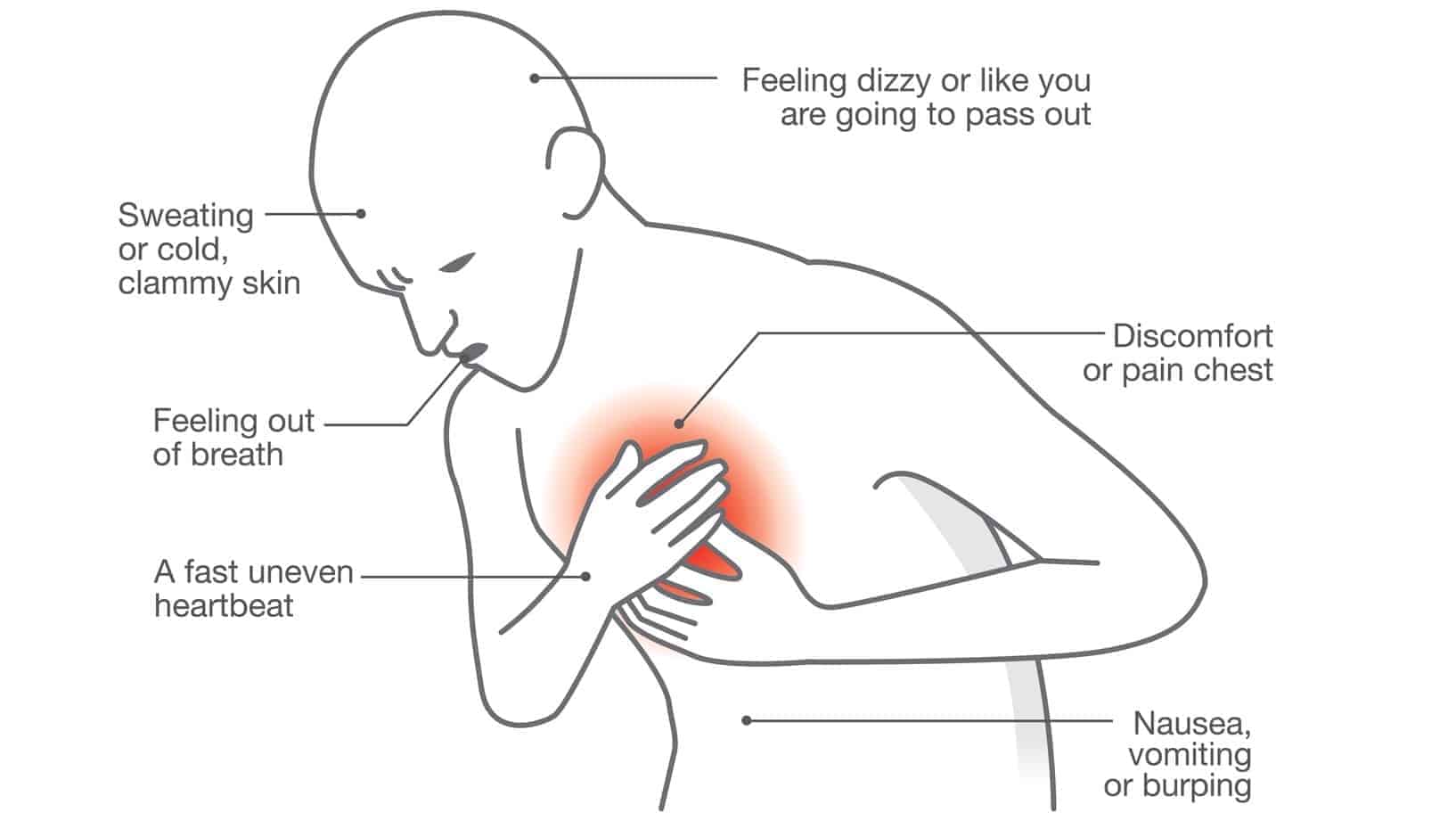
4. Heart attack.
It goes without saying, you must act immediately with this one. A “heart attack (also known as Myocardial infarction or MI), occurs when blood flow stops to a part of the heart causing damage to the heart muscle. The most common symptom is chest pain or discomfort which may travel into the shoulder, arm, back, neck, or jaw. Often it is in the center or left side of the chest and lasts for more than a few minutes. The discomfort may occasionally feel like heartburn. Other symptoms may include shortness of breath, nausea, feeling faint, a cold sweat, or feeling tired,” states Wikipedia.
However, the build-up of a heart attack “is normally gradual, over several minutes, and rarely instantaneous,” continues Wikipedia. The quicker you react to the onset of MI, the higher the chances of survival. Call emergency services immediately if you experience any of the mentioned symptoms.
5. Coronary heart disease, CHD.
Here are the causes of CHD, as described by NHS in the UK:
“Coronary heart disease is the term that describes what happens when your heart’s blood supply is blocked or interrupted by a build-up of fatty substances in the coronary arteries. Over time, the walls of your arteries can become furred up with fatty deposits. This process is known as atherosclerosis and the fatty deposits are called atheroma.
Atherosclerosis can be caused by lifestyle factors and other conditions, such as:
– smoking
– high cholesterol
– high blood pressure (hypertension)
– diabetes
Five Actions to Avoid Poor Heart Health and Live a Healthier Lifestyle
Avoiding poor heart health is something you can start doing today. Your lifestyle choices today benefit your heart healthy in the future. Here are five practical ways to keep your heart healthy.
1 – Eat a healthy heart diet
Eating healthy means you don’t eat from just one food group, but your diet includes a full range of natural foods from all the food groups, such as
- Whole grains-High in vitamins B and E.
- Fruits and vegetables- High in fiber, vitamins, and minerals
- Heathy fats-Olive oil and natural plant oils. This includes eating nuts and seeds.
- Eat low salt- High sodium diet isn’t good for your heart. Too much salt increases your risk of high blood pressure.
- Eat herbs and spices-Use these to flavor your food instead of salt or sugar
2 – Stay active
Regular exercise reduces your risk for a heart attack or heart disease. Exercise strengthens your heart, muscles, and bones. Staying active with exercise makes you feel happier and, depending upon the intensity of your exercise, it creates more neurons in your brain. It’s recommended that you do moderate exercise for at least 150 minutes a week. Some exercises you can do include
- Running
- Brisk walking
- Cycling
- Swimming
- Jumping rope
- Tennis
- Dancing
Doing something is better than nothing. Don’t feel overwhelmed at first. Set realistic goals for yourself. Start small and build up the time and intensity you’re exercising.
3 – Manage stress
Stress is a normal part of life, but if your stress is over the top, you need to manage it to keep your heart healthy. Add these things to your life to help reduce your stress.
- Exercise-Walk your dog, walk to your friend’s house instead of driving, take your kids on a hike.
- Take breaks-Take a personal day once a month to destress and get recharged.
- Slow down-Don’t allow busyness to rule your life.
- Find a hobby-Find a hobby. Do you love painting? Knitting? Dancing?
- Talk about your problems-Find a trusted friend to talk with about your problems.
4 – Know your cholesterol levels
Cholesterol is a fatty substance your body produces naturally. It’s also in foods. There are two types of cholesterol: good cholesterol (HDL) and bad cholesterol (LDL). Bad cholesterol builds up in your arteries, causing blockages that affect the blood flow to your heart. This puts you at risk for a heart attack or stroke. Eating too many “bad” fats found in fatty meats, pizza, pastries, or fried foods raises your cholesterol levels. Read labels on food packages and find healthy alternatives to avoid poor heart health.
5 – Regular Heart Health Check
Schedule a yearly check-up. Your health care provider will run tests to check your heart health. These include
- Blood pressure check
- Blood work to check your cholesterol levels
- Medical history information
Be sure to tell your doctor if you have symptoms that could show heart problems such as chest pains, dizziness, or fatigue.
Final Thoughts on Identifying the Signs of Poor Heart Health
Never ignore these five signs of poor heart health. Being aware of them could save your life. Taking care of your heart is something you can start doing right away. Healthy lifestyle choices such as regular exercise, eating natural, healthy foods, managing your stress, and regular check-ups will benefit your heart both today and in the future.
















 Community
Community

