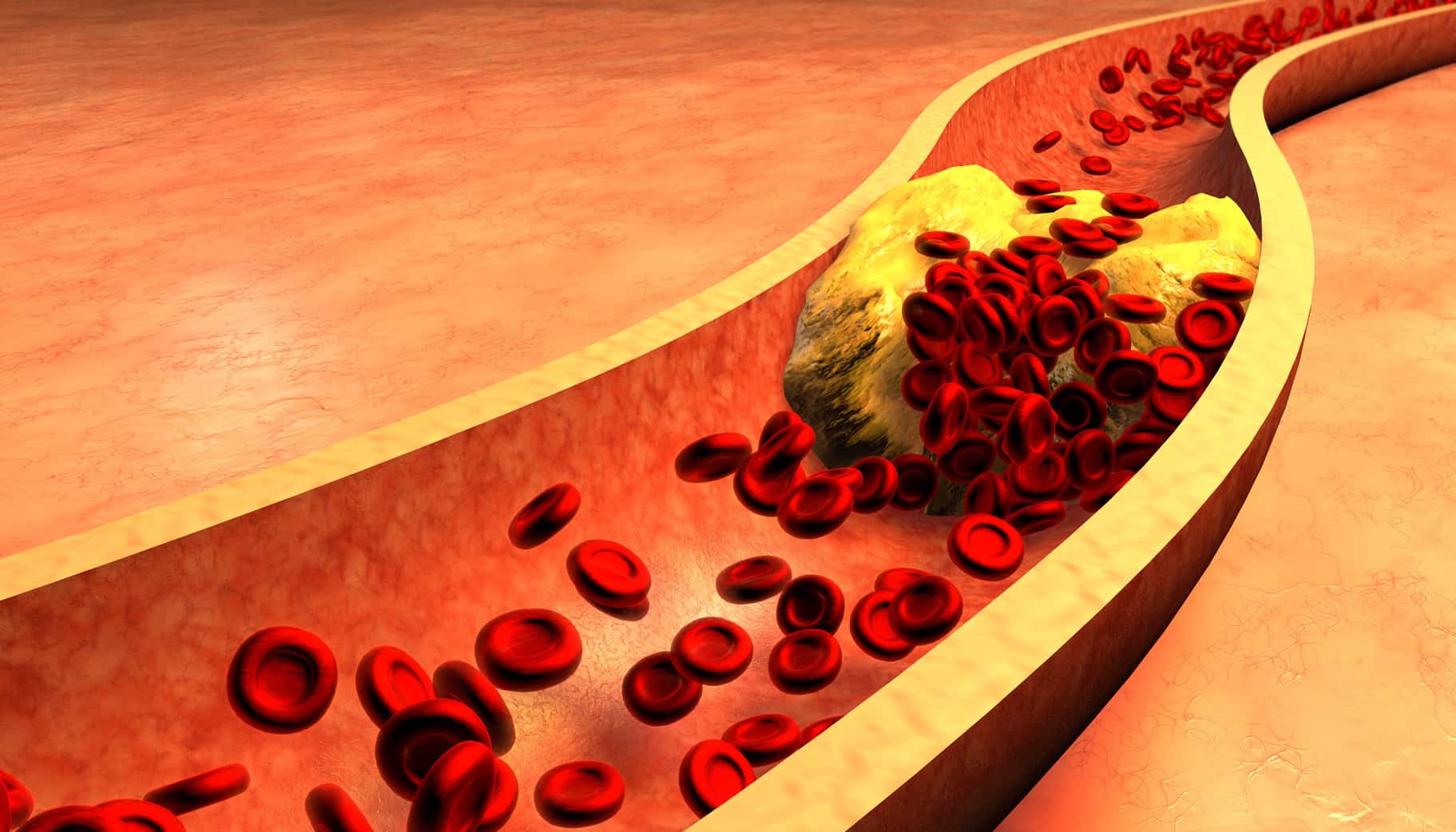
Atherosclerosis is a dangerous condition resulting from plaque deposits inside your arteries’ walls. This plaque buildup prevents delivering oxygen-rich blood to the heart, brain, and other vital body areas, potentially resulting in heart attack, stroke, or even death.
In advanced stages, atherosclerosis can be very difficult to treat. Before, the hardened plaque was nearly impossible to remove, and treatment was limited to risky procedures. The precarious areas where this buildup often limited available treatments and made the procedure more difficult.
However, this new technology can “eat” harmful arterial plaque and completely clean your arteries:
Then came the advent of a surgery called atherectomy (at-her-ec-toe-me), a minimally invasive procedure that can potentially treat advanced atherosclerosis. As opposed to traditional procedures, such as angioplasty and stents, atherectomy removes plaque buildup instead of simply moving or removing it.
A severe narrowing of the arteries must exist for someone to be a good candidate for the cutting-edge procedure. If not, traditional surgical methods such as angioplasty or stenting would be used. Further, bypass surgery must not be an option. In other words, atherectomy is a last resort, albeit probably the safest “last resort” procedure in history.
Doctors generally perform atherectomy when angioplasty or stenting is not an option. This determination is made with a few variables in mind – anatomical features, location of the blockage, or plaque hardness is usually a determinant. Atherectomy can also be used as a complementary procedure to traditional surgical methods, potentially increasing the odds of success.
How doctors perform this procedure that clears out the arteries
The fantastic aspect of this cutting-edge surgery is its intricacy and exactness – blood vessels and arteries are not very large. So, how can a tool that cuts away the material inside one be feasible? In a word: technology…in two more words: good doctor.
Once the patient is in the operating room, they receive a local anesthetic to numb the area being worked on. The patient is awake and sedated throughout the surgery.
Once sedated, the surgeon inserts a thin wire into the blocked artery via a needle inserted into a blood vessel in the groin. After this, the surgeon will insert dye into the artery while taking x-rays and observing while the dye continues to move through the body. These x-ray images give the surgeon the exact location to insert and maneuver the catheter.
The catheter inserted contains a cutting blade, grinding device, or laser filament used to remove the plaque. The device also contains a collection or suctioning system that effectively removes the debris. In some instances, the surgeon may opt to insert a stent at the location of the blockage to reduce the likelihood of another blockage.
Another remarkable aspect of this procedure is the healing time – 12 to 24 hours. Not days or weeks, as most surgeries generally require. A patient can usually continue with normal activity within a day or two.
Finally, doctors have seen tremendous results with the procedure. Very few risks exist for someone who opts for an atherectomy.
Here’s a video demonstrating the concept of the procedure:
The prolific threat from atherosclerosis is apparent when looking at the facts:
- It is the most common cause of cardiovascular diseases: heart attacks, strokes, and peripheral vascular disease
- Cardiovascular disease kills over 800,000 people annually, the most common cause of death.
Of course, preventative care is the best care. This is undoubtedly the case for atherosclerosis, an often deadly and debilitating disease. Good preventative care requires the determination of risk factors – the symptoms that often culminate in the surfacing of a severe condition.
Final thoughts on preventing atherosclerosis
Atherosclerosis is progressive but preventable. The disease’s nine risk factors account for approximately 90% of all heart attacks. These risk factors include the following:
- Smoking
- High cholesterol
- High blood pressure
- Diabetes
- Aging
- Inflammatory disease
- Family history of the disease
- Abdominal obesity
- Stress
- Not eating fruits and vegetables
- Excess alcohol intake
- Not exercising regularly
Once a blockage occurs, it is almost always permanent. Therefore, it is very important to mitigate potentially damaging consequences by making lifestyle changes. Of course, this condition mandates a healthy diet, regular exercise, and no smoking. While these changes will not eliminate the blockages, they can drastically lower the risk of heart attacks and strokes.











 Community
Community

